- Home
- Services
- About
- News
- Contact
- When did the song black beatles come ouy
- Microsoft office word 2013 free download windows 7
- Convert text to table word 7
- Lagu nasyid jagalah hati
- Tina casciani
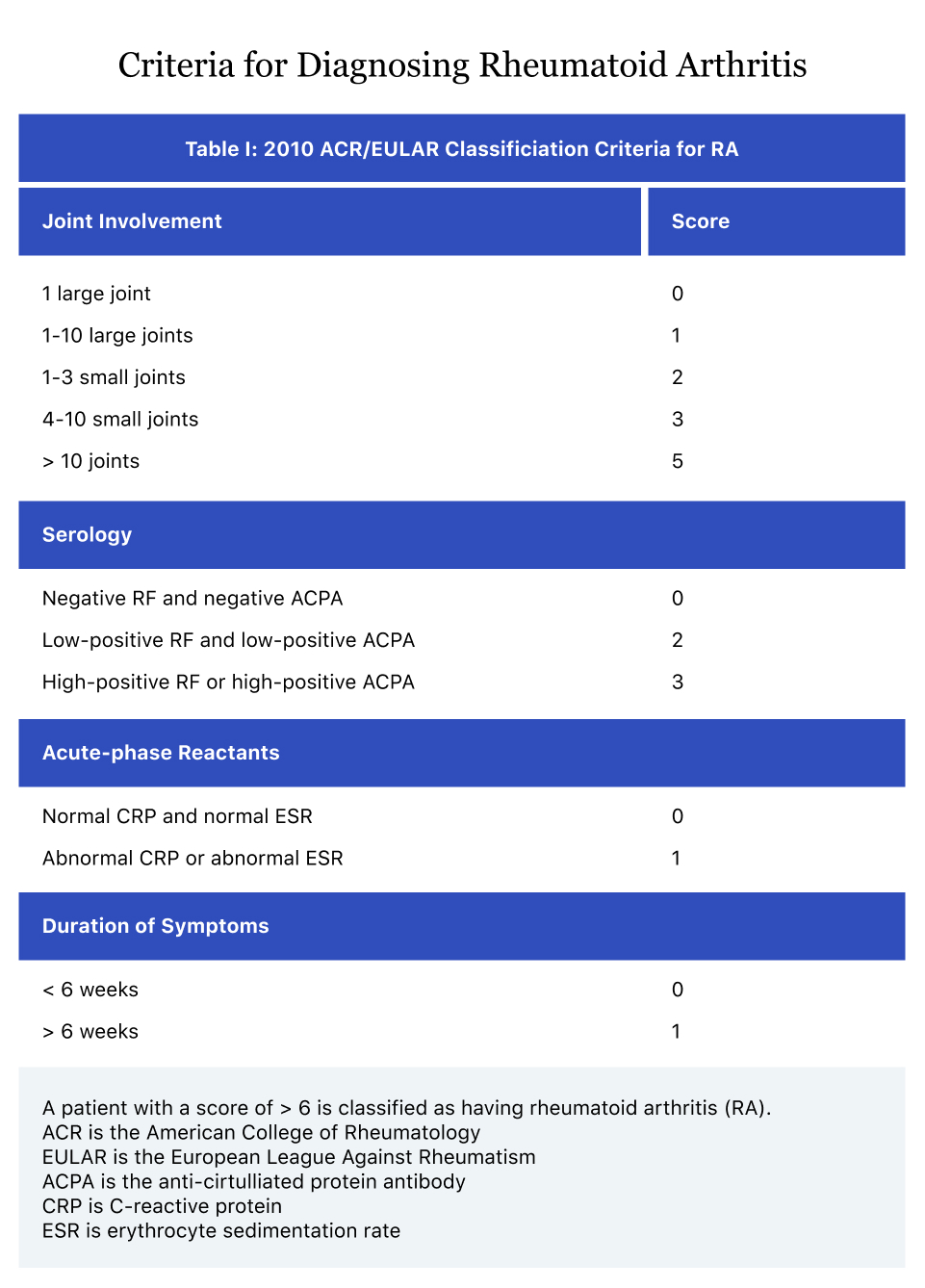
- Nqf rheumatoid arthritis diagnosis criteria
- Yin and yang symbol as moon and sun
- Vuze bittorrent client download
From the patient perspective, uncontrolled RA results in increased pain, fatigue, and reduced quality of life, affecting activity and the ability to work.

6 If properly controlled, RA can be manageable and exhibit periods of remission, 7 but uncontrolled RA can lead to involvement of other organ systems causing increased comorbidities and mortalities. RA is a chronic, inflammatory autoimmune disease primarily affecting the synovial joints. Therefore, quality of RA care, especially early in treatment when the disease course may be altered, is relevant to both patients and payers. 2–5 Due to the positive association between disease severity and higher health care costs, increased quality in health care could not only result in healthier patients, but reduce overall costs by slowing or mitigating disease progression. Conversely, increased patient involvement, initiation of proper treatment pathways, and timely interventions can aid patients in controlling chronic disease progression, thereby reducing the overall burden of disease on both the patient and health care system. 1 Patients with poorly maintained chronic diseases can further increase these cost burdens because of augmented use of health care services. Yet, the overall cost of RA care is likely to remain high because of intensive pharmacotherapy regimens.Ĭ hronic diseases such as rheumatoid arthritis (RA) represent a large burden on health care systems because of increased use of services over time. These findings suggest that increased quality may lead to lower inpatient and outpatient hospital costs. Individuals meeting the measures had a higher proportion of costs accounted for by office visits those not meeting the measures had a higher proportion of costs from inpatient and outpatient visits. Pharmacy costs were similar between both groups. Regression analyses revealed statistically significant associations between biologic usage, which was more prevalent in groups attaining measures, and total expenditure across all measures ( Ps < 0.001).
#Nqf rheumatoid arthritis diagnosis criteria drivers
Primary cost drivers were pharmacy and office expenses, accounting for 42.4% and 26.3% of total costs, respectively. The mean cost of care for members meeting the measure was $18,644 members who did not meet the measures had a mean cost of $14,973. Measure achievement ranged from 55.9% to 80.8%. Individuals were predominately female and in their mid-fifties.
Medical, pharmacy, and laboratory claims for RA patients ( International Classification of Diseases, Ninth Revision, Clinical Modification 714.x) were extracted from the Optum Clinformatics Datamart database for 2011. Associated health care costs were calculated for members who achieved or did not achieve each of the measures. Administrative claims were used to calculate 8 process measures for the treatment of RA. The objective was to examine the relationship between health care costs and quality in rheumatoid arthritis (RA).
- Home
- Services
- About
- News
- Contact
- When did the song black beatles come ouy
- Microsoft office word 2013 free download windows 7
- Convert text to table word 7
- Lagu nasyid jagalah hati
- Tina casciani
- Nqf rheumatoid arthritis diagnosis criteria
- Yin and yang symbol as moon and sun
- Vuze bittorrent client download
